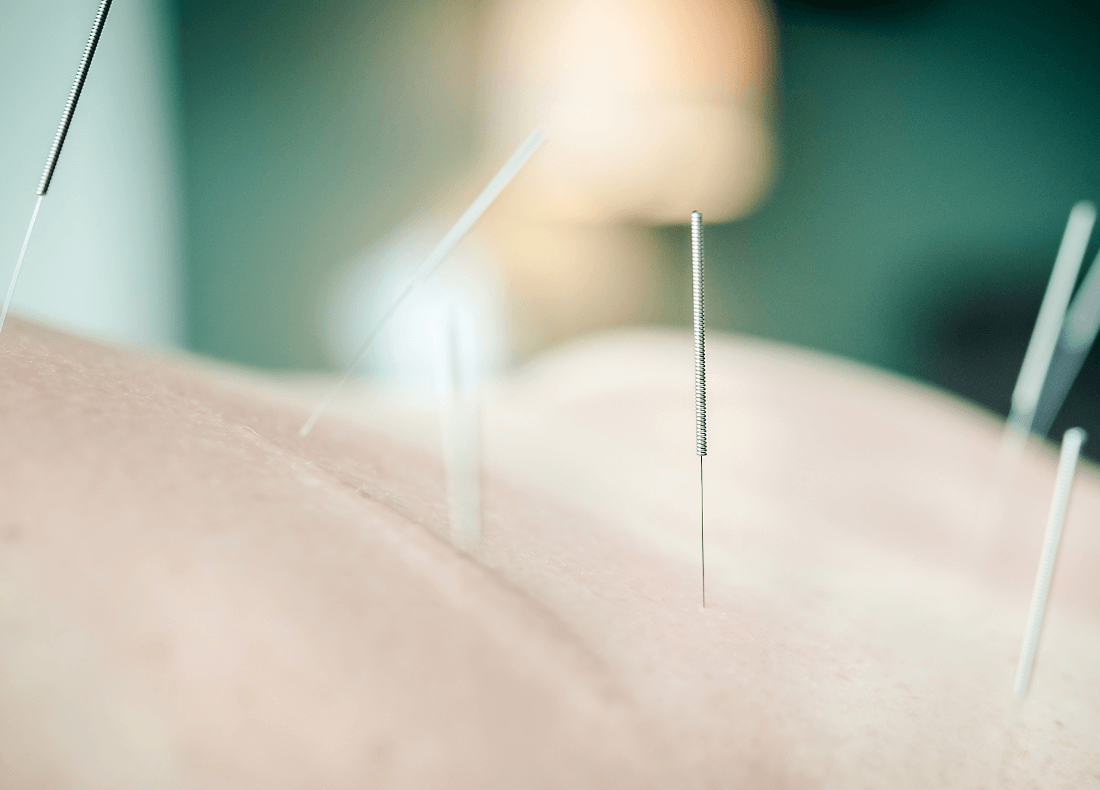
IMS/Dry Needling
Getting to the point
IMS, also known as Dry Needling, can be a game-changer for people dealing with musculoskeletal issues or nerve pain.
Our Customer Reviews
What is IMS/Dry Needling?
Intramuscular Stimulation (IMS), also called dry needling, is a treatment that involves inserting a fine needle into muscle to address pain, tenderness, and movement limitation associated with myofascial trigger points or altered muscle tone without injecting medication. Research suggests it may help reduce pain and improve short-term function for some musculoskeletal conditions, especially when it is combined with an active rehabilitation plan.
The terms “IMS” and “Dry Needling” are often used interchangeably in clinical settings, although terminology can vary by region and training background.
How can IMS/Dry Needling help?
Dry needling is thought to influence pain through several mechanisms, including changes in local muscle sensitivity, trigger point irritability, and modulation of pain processing. Systematic reviews show that dry needling can reduce pain and improve pressure pain threshold in the short term, with the best evidence for immediate to 12-week benefits.
Does Research Support the Use of IMS/Dry Needling?
Evidence for dry needling is strongest for certain musculoskeletal pain presentations rather than for every diagnosis. A 2017 systematic review and meta-analysis found that dry needling performed by physiotherapists was more effective than no treatment, sham needling, or some other treatments for reducing pain and improving pressure pain threshold in the short term, but evidence for long-term benefit was lacking. A newer umbrella review also concluded that dry needling is generally superior to sham or no intervention for short-term pain reduction, while being similarly effective to other interventions for pain relief in the short term.
What Conditions does IMS/Dry Needling Treat?
Studies and systematic reviews report potential benefit in neck pain, shoulder pain, low back pain, and some tendinopathy-related conditions, especially when pain is driven by myofascial trigger points or when it is used alongside exercise and other physiotherapy care.
For chronic neck pain, more recent meta-analytic evidence suggests dry needling can improve pain and function in the short to mid term, though the overall evidence base still supports a careful, individualized approach rather than a one-size-fits-all promise. For low back pain, systematic reviews suggest dry needling may help pain, especially when combined with other therapies, but evidence for disability improvement is less consistent.
Is it Safe?
Dry needling is generally considered low risk when performed by a trained clinician using proper screening and sterile technique. The most common side effects are mild and temporary, including bleeding, bruising, soreness, or discomfort during treatment.
Serious adverse events are very rare, but they can occur, which is why anatomy, informed consent, and clinical judgment matter. Reported serious risks include infection and pneumothorax, but these cases were usually the result of severe carelessness by the practitioner.
What to Expect
A typical session begins with an assessment of your symptoms, movement, and relevant tissues so the treatment matches your goals. If dry needling is appropriate, a fine needle is inserted into the targeted tissue and may be left briefly or gently moved around at different angles depending on your physiotherapist’s approach and your response.
You may feel a quick pinch, twitch, ache, or pressure during treatment, and mild post-treatment soreness can last for a short period afterwards. Dry needling is often paired with exercise, manual therapy, and education around load management so improvements translate into better daily function.
Who May Benefit?
Dry needling may be appropriate if your pain appears to be driven by muscular trigger points, persistent muscle tightness, or pain that is limiting rehab progress. It may be especially useful when symptoms are stopping you from loading, strengthening, or moving normally.
It is not the best choice for every person, and it is rarely the only treatment needed. The best outcomes are generally seen when dry needling is used as part of a broader plan that addresses strength, mobility, workload, and the source of the problem.
If it’s the right fit for you, we include IMS/dry needling as part of our treatment sessions at no additional cost.
Who Performs IMS/Dry Needling?
This service is offered by our registered physiotherapists who are also certified dry needling practitioners – Mary-Anne Levson, Nina Bai, Roman Zaliskyy, Cathy Stedman, and Evan Thomas.
References
- Gattie E, Cleland JA, Snodgrass S. The Effectiveness of Trigger Point Dry Needling for Musculoskeletal Conditions by Physical Therapists: A Systematic Review and Meta-analysis. J Orthop Sports Phys Ther. 2017; 47(3): 133-149.
- Solomons L, Lee JJY, Bruce M, White LD, Scott A. Intramuscular stimulation vs sham needling for the treatment of chronic midportion Achilles tendinopathy: A randomized controlled clinical trial. PLoS One. 2020; 15(9): e0238579.
- Chys M, De Meulemeester K, De Greef I, Murillo C, Kindt W, Kouzouz Y, Lescroart B, Cagnie B. Clinical Effectiveness of Dry Needling in Patients with Musculoskeletal Pain-An Umbrella Review. J Clin Med. 2023; 12(3): 1205.
- Liu L, Huang QM, Liu QG, Ye G, Bo CZ, Chen MJ, Li P. Effectiveness of dry needling for myofascial trigger points associated with neck and shoulder pain: a systematic review and meta-analysis. Arch Phys Med Rehabil. 2015; 96(5): 944-55.
- Brady S, McEvoy J, Dommerholt J, Doody C. Adverse events following trigger point dry needling: a prospective survey of chartered physiotherapists. J Man Manip Ther. 2014; 22(3): 134-40.
- Hu HT, Gao H, Ma RJ, Zhao XF, Tian HF, Li L. Is dry needling effective for low back pain?: A systematic review and PRISMA-compliant meta-analysis. Medicine (Baltimore). 2018; 97(26): e11225.
- Hall ML, Mackie AC, Ribeiro DC. Effects of dry needling trigger point therapy in the shoulder region on patients with upper extremity pain and dysfunction: a systematic review with meta-analysis. Physiotherapy. 2018; 104(2): 167-177.
- Nuhmani S, Khan MH, Ahsan M, Abualait TS, Muaidi Q. Dry needling in the management of tendinopathy: A systematic review of randomized control trials. Journal of Bodywork and Movement Therapies. 2022; 33, 128-135.

